| |
Atopic dermatitis, also known as atopic eczema, is a chronic, relapsing inflammatory skin condition. It is a very common disorder, affecting approximately 20% of children and 2–8% of adults. It usually appears during infancy or early childhood, and in most cases it resolves before adolescence. However, a significant proportion of adults may develop the condition for the first time later in life.
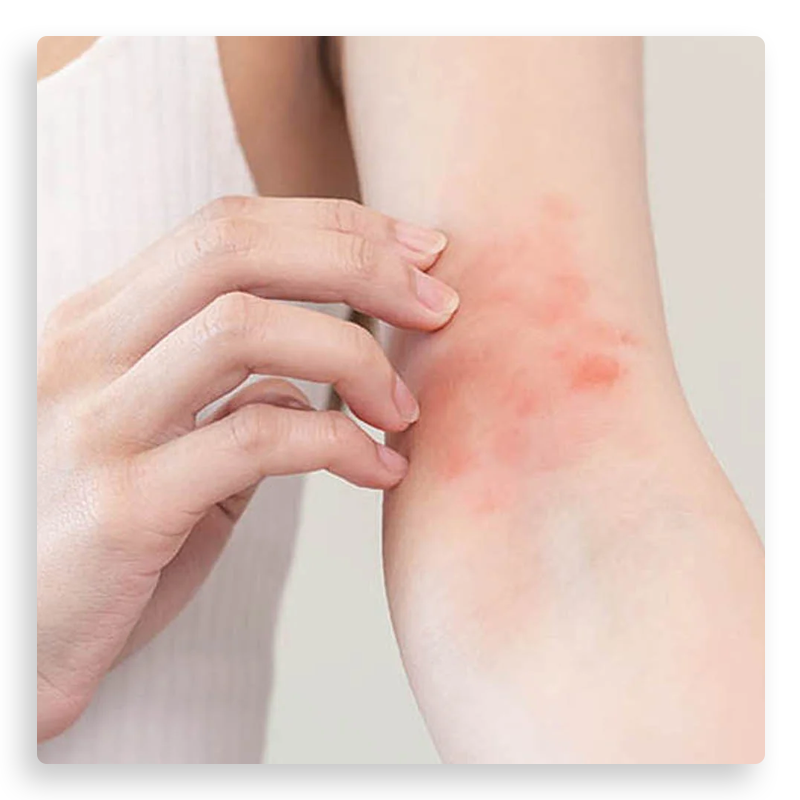
The cause of atopic dermatitis is complex, as it is linked to the interaction between genetic and environmental factors. This interaction leads to the manifestation of various clinical forms of the disease. Although the exact mechanism is not fully understood, it appears to involve dysfunction of the skin barrier, abnormal lipid metabolism of the epidermis, and increased sensitivity of the immune system to allergic reactions. This results in overproduction of immunoglobulin E (IgE) to various allergens, without necessarily leading to clinically evident allergic diseases.
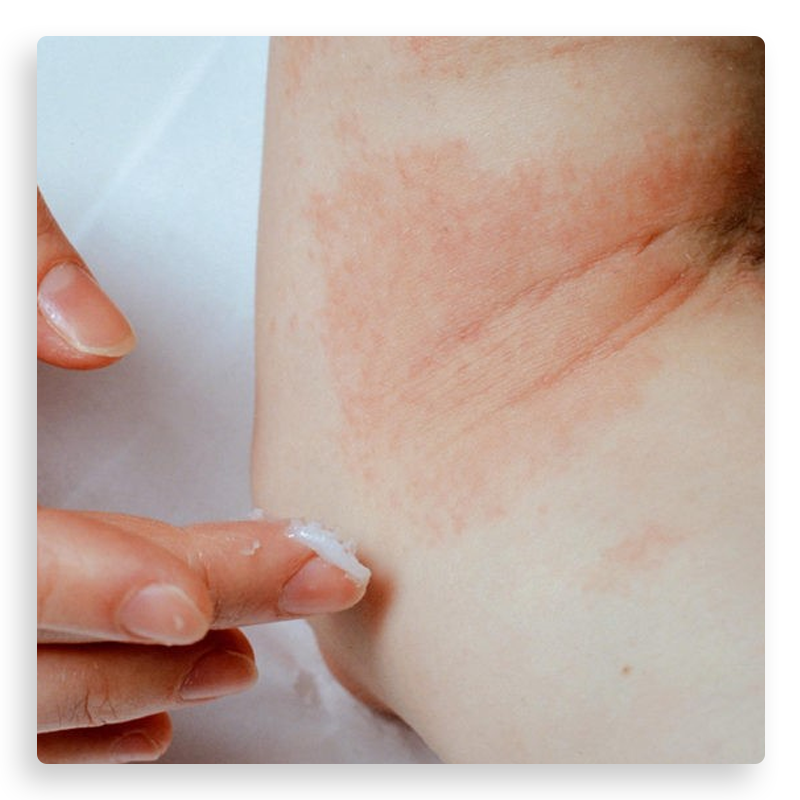
The course of atopic dermatitis is chronic, characterized by periods of remission and flare-ups of varying severity. During remission, the skin is dry and rough with mild itching, while during flare-ups there is intense itching, redness, small blisters, and possibly oozing. Without treatment, inflammation may worsen, leading to skin erosion. In infants, lesions are usually located on the face, while in children they commonly appear in skin folds such as behind the knees, elbows, wrists, and neck.
Relapses are often triggered by irritants such as cold, sweat, dust, friction, and stress. The itching leads to scratching, which damages the outer layer of the skin, allowing irritants and allergens to penetrate. This further intensifies inflammation and creates a vicious cycle of itching and scratching, often worsening at night.
|
Atopic dermatitis is often the first manifestation of allergic diseases, with others such as food allergy, rhinitis, and asthma appearing later. However, this does not mean that all children with atopic dermatitis will develop other allergies. The allergist evaluates possible allergic sensitization and its relationship to the course of the disease. Although many children show positive skin tests or RAST tests, positive results do not necessarily indicate an allergic condition. It is important to avoid unnecessary dietary restrictions without clear indication.
Proper information and education of patients or parents about the nature of the condition is essential. Moisturization is a key component of treatment, while the correct use of topical or systemic medications helps in effective disease management. Cooperation and trust between doctor and patient contribute to improving quality of life, reducing flare-ups, and promptly addressing any associated allergic conditions.
| |
|
Treatment
Treatment of atopic dermatitis aims to manage symptoms, prevent flare-ups, and improve patients’ quality of life. It is based on a combination of strategies including skin care, medication, and avoidance of triggering factors.
Skin hydration is the foundation of treatment and the most important step in maintaining the skin barrier function. Regular use of special moisturizing products (emollients) is recommended to prevent dryness. They should be applied immediately after bathing to “lock in” moisture.
During flare-ups, topical anti-inflammatory medications such as corticosteroids or calcineurin inhibitors (e.g., tacrolimus and pimecrolimus) are used to control inflammation and itching. Topical corticosteroids are selected based on disease severity and application area, and their use should be monitored by a physician to avoid side effects.
|
| |
| |
|
|
|